Over the past few months, much of Asia – like many other parts of the world – has returned to an uncanny normality. Streets are full of people, schools and universities are open, traffic is jamming the roads, shops are bustling and there is little, if any, social distancing. COVID-19 restrictions have been lifted across most Asian countries, with mask mandates and minor restrictions on international travel the common thread that reminds us of the past two and a half years.
Looking back, it might have been a lot worse for many of Asia’s poorer countries. Much of Asia – including India, Indonesia, the Philippines and Vietnam – falls into what the World Bank categorises as ‘lower-middle income countries’ (LMICs), where citizens earn on average between US$1,000 and US$4,000 per year. Despite their cultural, social and political diversity, Asia’s LMICs share several governance challenges, particularly around institutional capabilities, quality of policymaking and implementation, and the quality of services delivered to citizens.
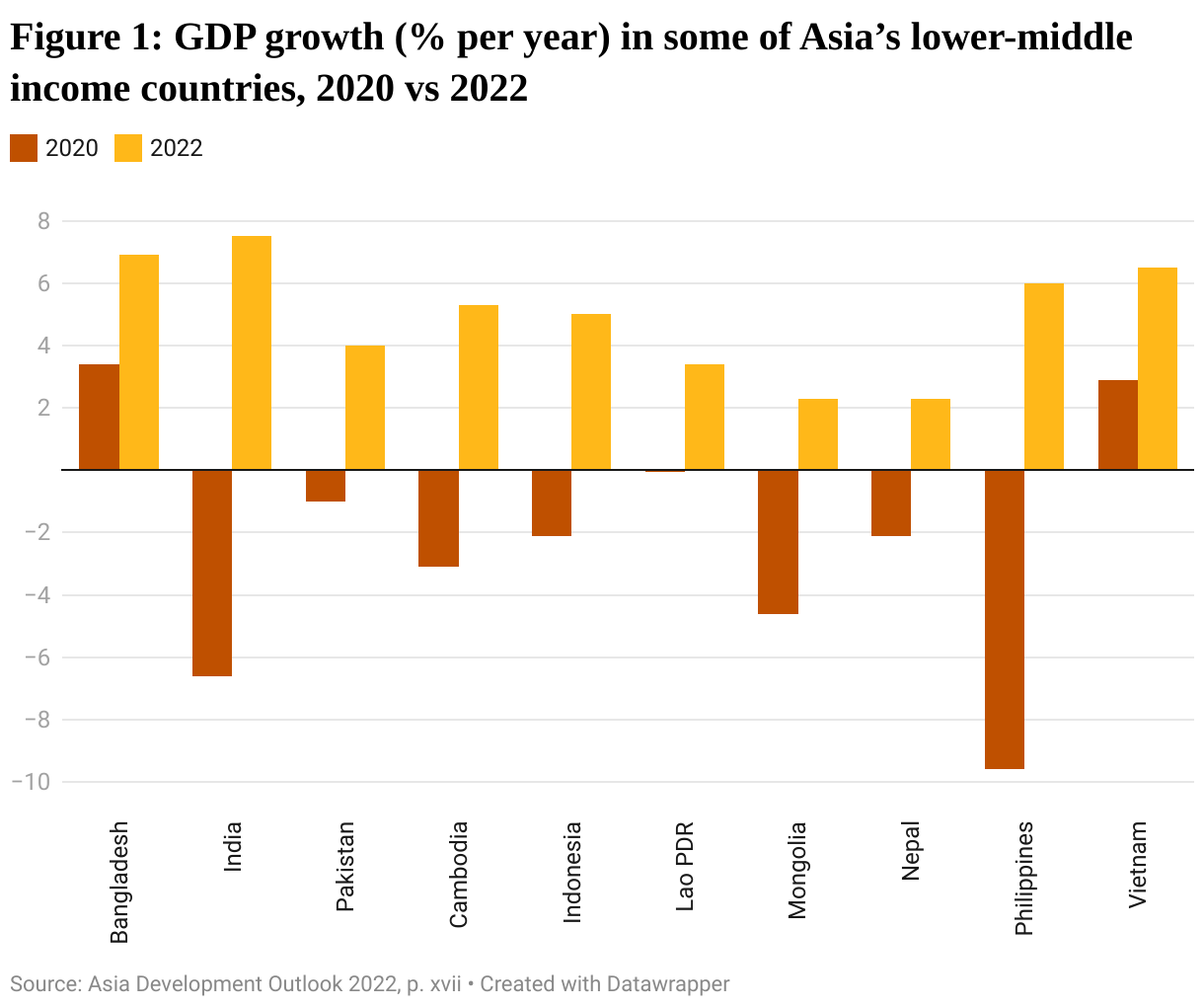
While the economic shock of COVID-19 across Asia was immense – with over 9 million jobs lost and 4.7 million people pushed below the poverty line in Southeast Asia alone – much of the region is bouncing back with verve. Estimates from the Asian Development Bank and others foresee a return to economic growth across the region after the slump of 2020 and 2021.
A central driver has been the generally very well orchestrated, government-led vaccination programs. At the time of writing, 72% of the region’s population have completed the initial vaccine protocol, compared with 67.5% in the United States and 66.2% in the European Union. Once they secured vaccine supplies, governments moved swiftly and efficiently to get them to citizens.
In our most recent issue of GovAsia – ‘Rollout: Reflections on COVID-19 vaccination programs in lower middle income Asia‘ – we look at how governments managed massive vaccination campaigns in much of LMIC Asia in 2021. Notwithstanding the enormous social, cultural and political differences between countries like India and Laos, or Pakistan and Vietnam, we found some commonalities in the successes and challenges they faced in rolling out the vaccination programs.
First, deep inequities in the global distribution of vaccines in 2021 caused shortages in all but the wealthiest countries, the knock-on effects of which were significant. These were largely due to patent restrictions, which meant that only India was able to produce vaccines internally, while other Asian LMICs were left to rely on imports. After much of the global supply was purchased, with countries such as Canada procuring several times more than required to meet their population needs, a waiting game set in across the region from early to mid-2021. For some countries, such as Vietnam, it was not until the end of the year that the supply of vaccines started to keep pace with demand.
Second, most LMICs experienced difficulties in national rollout programs due to a combination of factors, such as elite capture of vaccinations, under-the-counter distribution, unclear policies, and a lack of national and local government coordination. These challenges were compounded by corruption scandals across the region that damaged public trust and contributed to an inequitable distribution of vaccines. In Nepal, a scandal over the procurement of vaccines led to a halt of the vaccine rollout in January 2021, leaving some people partially vaccinated and many more without any vaccines at all.
Third, several LMICs struggled to administer vaccinations equitably and efficiently, despite having all identified priority groups early in their campaigns. As 2021 wore on, the tendency to prioritise economic considerations over health concerns grew stronger, and further inhibited the efficiency of vaccination campaigns. In Indonesia and India, rural communities were vaccinated at a notably slower pace due to a range of issues including lower levels of smartphone access, digital illiteracy, poor internet connectivity and vaccine hesitancy.
And lastly, several LMICs have faced some degree of vaccine hesitancy, although notably nowhere close to the extent of the anti-vax movements experienced elsewhere in the world. In India, Nepal and the Philippines, mRNA vaccines were initially considered safer than non-mRNA vaccines, especially those in the latter category produced by China. This made it difficult for Asian LMIC governments in 2021, when only non-mRNA vaccines were available. Across the board, vaccine hesitancy was largely caused by the spread of disinformation across social and other media platforms.
Many challenges persist as vaccine programs continue in Asian LMICs. These are underpinned by a suite of governance challenges, including corruption, failure to strengthen broader health system capacity, and poor coordination among national and local government agencies, civil society, the private sector, and other actors.
COVID-19 response efforts have pointed to a combination of priority local, regional and global actions that will ensure Asian LMICs are better prepared for future pandemics or other major challenges.
The pandemic has made it abundantly clear how low and lower-middle income countries need quality universal health systems, with strong emergency response capacity, underpinned by efficient and effective government systems and structures. In addition, there needs to be more investment in the local production of anti- and long-COVID treatments, and measures taken to increase access to digital health services, particularly for marginalised and disadvantaged groups.
In the momentum for collaboration generated by the pandemic, there are opportunities for regional knowledge and technology sharing on pandemic management and health system strengthening. At the same time, there is more to be learnt from the experience – both successes and challenges – of Asian LMICs, some of which consistently outperformed wealthier countries and regions in their response to the pandemic, including vaccine rollout.
The upcoming G20 meeting in December 2022 is an important opportunity to strengthen solidarity regionally and internationally. Where efforts to improve global pandemic preparedness and response are already on the table, these must take into account not only the improved testing and therapies, research and development, manufacturing and health infrastructures needed to combat COVID-19 or future pandemics, but also the characteristics of the governance contexts in which measures will be implemented, and the underlying systemic challenges which also need to be addressed.
This post is part of a collaborative series with The Asia Foundation.







