Much has been made of Australia’s 2025–26 Official Development Assistance (ODA) budget. At $5.097 billion, it marks a slight nominal increase from prior years yet continues to shrink in real terms. The aid-to-gross national income (GNI) ratio is now at a historic low of 0.18%, and even before that, in 2024, Australia sat at 28th out of 33 donor countries in the Organisation for Economic Co-operation and Development (OECD) — firmly among the least generous contributors.
While the spotlight stays fixed on these topline figures, beneath the surface lies a deeper emerging issue. Health, once a cornerstone of Australia’s development program, is being quietly pushed to the margins, not just in terms of overall funding but through a steady retreat from long-term investments in health systems strengthening.
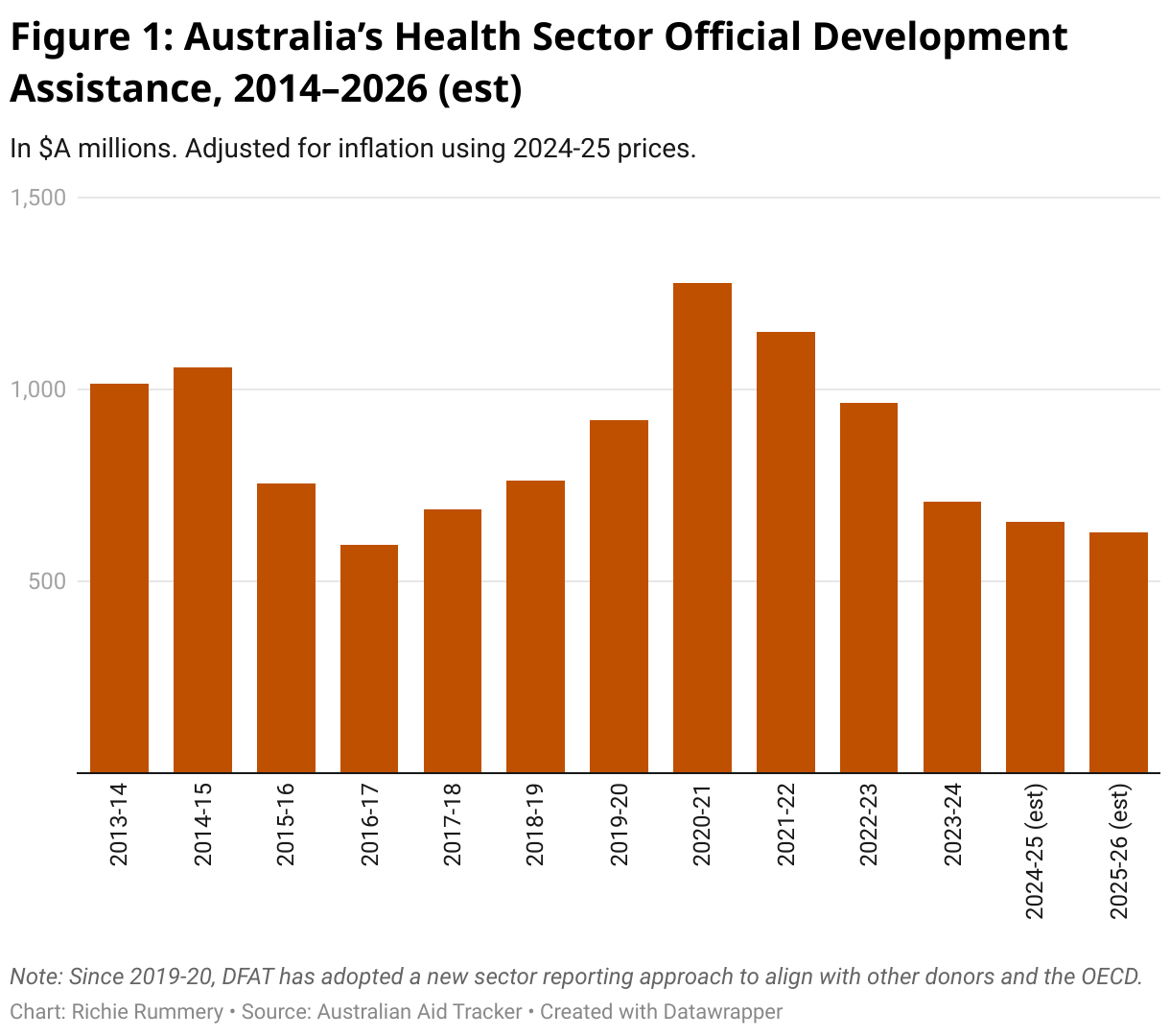
Based on currently released budget allocations, funding is set to fall to just $628 million, effectively halving Australia’s health aid in five years. While this drop can be partly rationalised by reference to the COVID-19 response that temporarily boosted health aid to record levels, the more concerning trend is the sustained decline compared to pre-pandemic investment levels. Health aid is expected to fall by 40% from its 2014–15 level, signalling that long-term support for health is slipping further down the aid agenda.
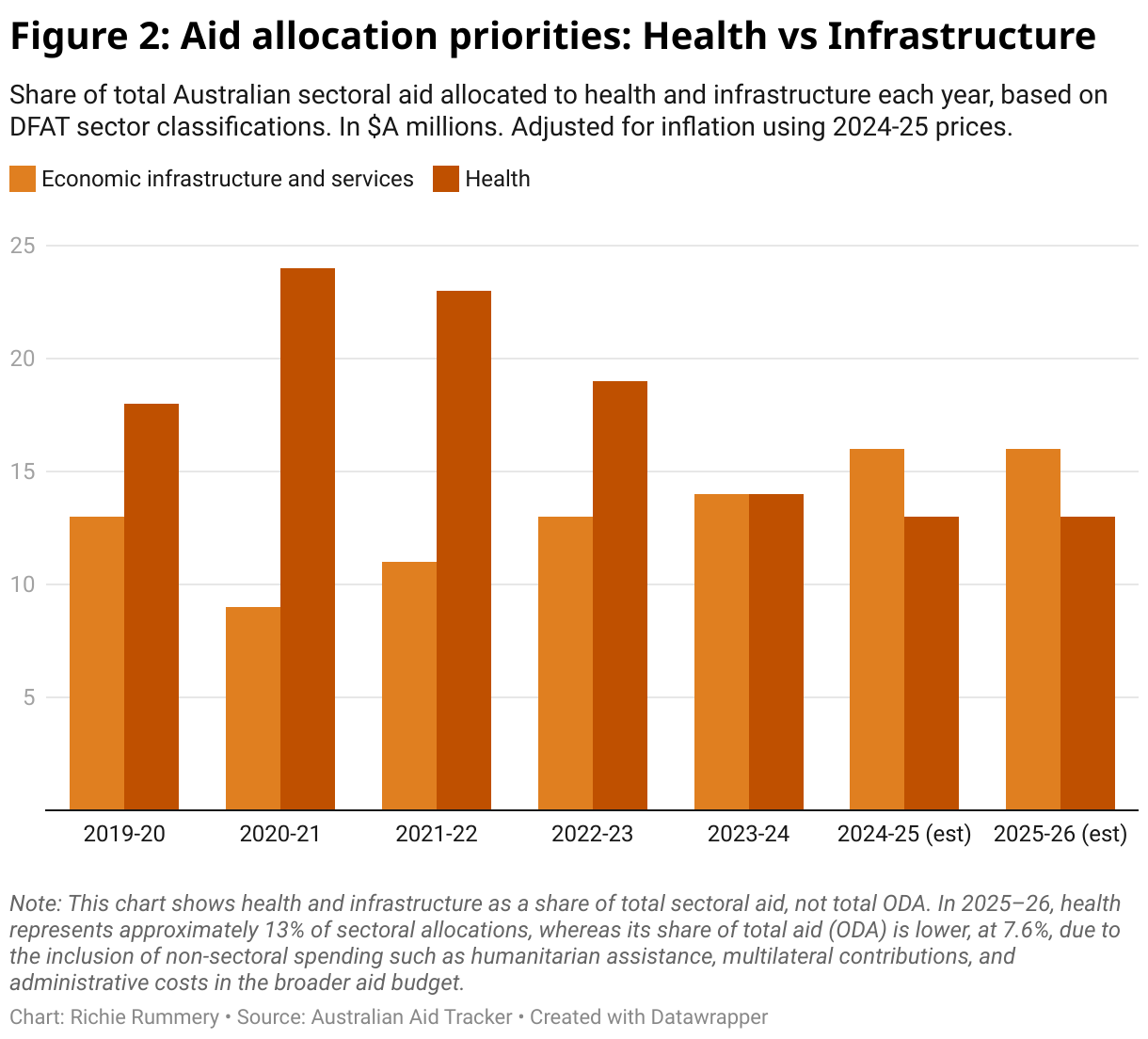
This is not a trend unique to Australia. ODA for health from OECD countries is projected to drop by 40% in 2025. While health was once a central priority for sovereign donor programs, recent aid budgets suggest a shift away from health and toward areas deemed more aligned with geostrategic interests. In Australia, this trend is demonstrated by recent shifts in sectoral aid allocations. While the share of aid allocated to health has steadily declined, the proportion directed to economic infrastructure has grown. This reflects a broader reordering of Australia’s aid priorities toward visibility, strategic return and geopolitical advantage.
This overall decline in health aid has been particularly damaging for health systems strengthening (HSS) — that is, efforts to improve the performance of health services through integrated, system-wide reforms. The World Health Organization (WHO) groups these systems into the core health building blocks of service delivery, workforce, information, medicine access, financing and governance — foundational elements that take years to strengthen because they require incremental institutional change, capacity development and sustained political commitment.
However, HSS is being increasingly deprioritised across the spectrum of OECD countries, often because impact is difficult to measure and investments can be slow to deliver results. This retreat reflects a broader reorientation of the purpose and politics of health-related development assistance. In Australia, there is growing pressure to align aid more closely with the national interest. This has led to increasing investments in infrastructure, disaster recovery and security cooperation — areas that offer visibility and strategic influence but often at the expense of long-term development objectives. HSS often sits uneasily within Australia’s current foreign policy-driven aid agenda as it is less likely to deliver short-term wins or the diplomatic leverage that high visibility infrastructure enables. But that does not make it any less strategic.
On the contrary, resilient health systems are a foundation for stability. When health systems fail, the human, economic and political costs are glaring. When they work well, they tend to operate quietly in the background, supporting populations to remain healthy, slowly lowering disease burdens, preventing outbreaks, enabling productivity in education and employment and promoting societal cohesion. Their success is measured in terms of the quiet absence of avoidable crisis. Yet, this “under the bonnet” approach leaves HSS easily forgotten behind the façade of high-impact aid. Arguably, this is short-sighted. Without resilient systems in place, the next health shock, whether local or global, will again expose the fragility that underinvestment has left, leaving development programs scrambling to plaster over what could have been built to endure.
In the Pacific, the consequences of neglecting health systems are already apparent. Health systems remain fragile, under-resourced and overburdened, pressured not only by the rising double burden of communicable and non-communicable diseases, but also by broader structural vulnerabilities that lead to service delivery crises and leave health systems ill-equipped to respond to public health emergencies. Australia has long played a leadership role in supporting HSS across the region and, in the wake of the recent USAID closure, arguably now has an even greater responsibility. The Australian government’s five-year Partnerships for a Healthy Region Initiative (2022–23 to 2026–27) marks a welcome shift in regional health aid, moving beyond a narrow focus on infectious diseases to include broader health system resilience. However, its limited timeframe is ill-suited to the deep, sustained reforms that health systems strengthening demands.
These longer-term, systemic efforts have traditionally been driven by Australia’s bilateral health programs. Yet in an increasingly complex and contested development landscape, the trajectory of bilateral health aid points in the opposite direction. A pre-COVID-19 independent review of Australia’s bilateral health investments in the Pacific found real, incremental improvements in areas such as workforce capacity, information systems, governance and medical supply chain management. Crucially, the review concluded that without sustained investment in HSS, those gains would stall or reverse. Rather than stepping back, it recommended doubling down on HSS as the only viable path to making lasting progress toward universal health coverage targets.
Today, that warning feels more urgent than ever, as the steady gains of the past start to unravel. In the years since that evaluation, the COVID-19 pandemic, numerous regional natural disasters and a shifting geopolitical landscape have tested the resilience of health systems across the Pacific. Yet, Australia’s bilateral aid programs have increasingly pivoted away from long-term HSS reform. Bilateral health funding has declined in real terms, and the balance of investment has tipped toward infrastructure and other high-visibility initiatives. The momentum behind HSS, once a cornerstone of regional engagement, is in danger of being forgotten — buried beneath bricks and mortar, band-aid investments and political optics.
If Australia’s health-for-development agenda is to retain credibility and effectiveness in the Pacific, it must restore the balance between responsiveness and reform. Infrastructure has its place among the many levers development programs can pull to support Pacific health ministries, but it must not be allowed to crowd out the policy engagement, institution-building and leadership development that underpins HSS and expanded universal health coverage. None of this requires abandoning national interest; in fact, the opposite is true. Supporting regional health systems is very much in Australia’s national interest as it helps create the kind of secure, prosperous neighbourhood that meaningful diplomacy also seeks to foster.
Whether this view will regain prominence in the years ahead remains to be seen. For now, health is slipping from the radar, and with it, the quiet architecture of resilience that holds steady in the face of crisis. What’s being lost is not just funding or an HSS focus but, more concerningly, the appetite for the long game.








Insightful read! Thank you Richie for putting this together, as a young Papua New Guinean interested with the Economics of Health and International development, this gives me much needed perspective.
A challenge for us Pacific Island nations would taking control of our development agenda, this would mean setting our priorities and putting health front and center in our development plans. I’ve been reading about investments in Defense treaties and sports diplomacy all while health takes a back seat. I hope we will see a shift in momentum towards HSS in the years to come.
A very interesting and informative blog. Recent international reports add to those concerns, shedding light on gaps and weaknesses in underlying health systems. For example, the latest Sustainable Development Report 2025, available here, finds on page 23 that none of the 21 countries in East and South Asia are “on track” to achieve Sustainable Development Goal (SDG 3) which targets “good health and wellbeing”. The report also finds that 14 countries in that region face “major challenges” and 5 face “significant” challenges in achieving SDG 3 by 2030. The report also finds (page 26) that none of the 12 Pacific Island countries are “on track” to achieve SDG 3; all 12 have “major challenges” in achieving SDG 3; that 7 countries are “stagnating” and the remaining 5 are only “moderately increasing” progress to achieving SDG 3.
Furthermore, the World Bank and World Health Organization separately report that “The world is off track to make significant progress towards universal health coverage (UHC) by 2030 as improvements to health services coverage have stagnated since 2015, and the proportion of the population that faced catastrophic levels of out-of-pocket (OOP) health spending has increased….Moreover, the majority of countries (108/194) experienced worsening or no significant change in service coverage since the launch of the SDGs in 2015” (Source: Tracking universal health coverage: 2023 global monitoring report, page xi and xii).
Thanks Ian, really appreciate you taking the time to read and share those stats. I hadn’t seen the latest Sustainable Development Report but those figures paint a pretty stark picture. It’s hard to argue we’re on the right trajectory when no country in the Pacific is on track for meeting SDG 3.
Also, I have to give credit where it’s due. The phrase “under the bonnet” in the article was one I borrowed from you in your description of the Health Sector Support Program in Solomons a few years ago. I always thought it perfectly captured the nature of HSS focused programs.
Thanks again.