While Australia gradually reopens to the world, some of its closest Pacific neighbours are still struggling with low COVID-19 rates of vaccination and new waves of infection. But after two years of lessons learnt fighting the global pandemic, governments across the region are better armed to improve rates of vaccination.
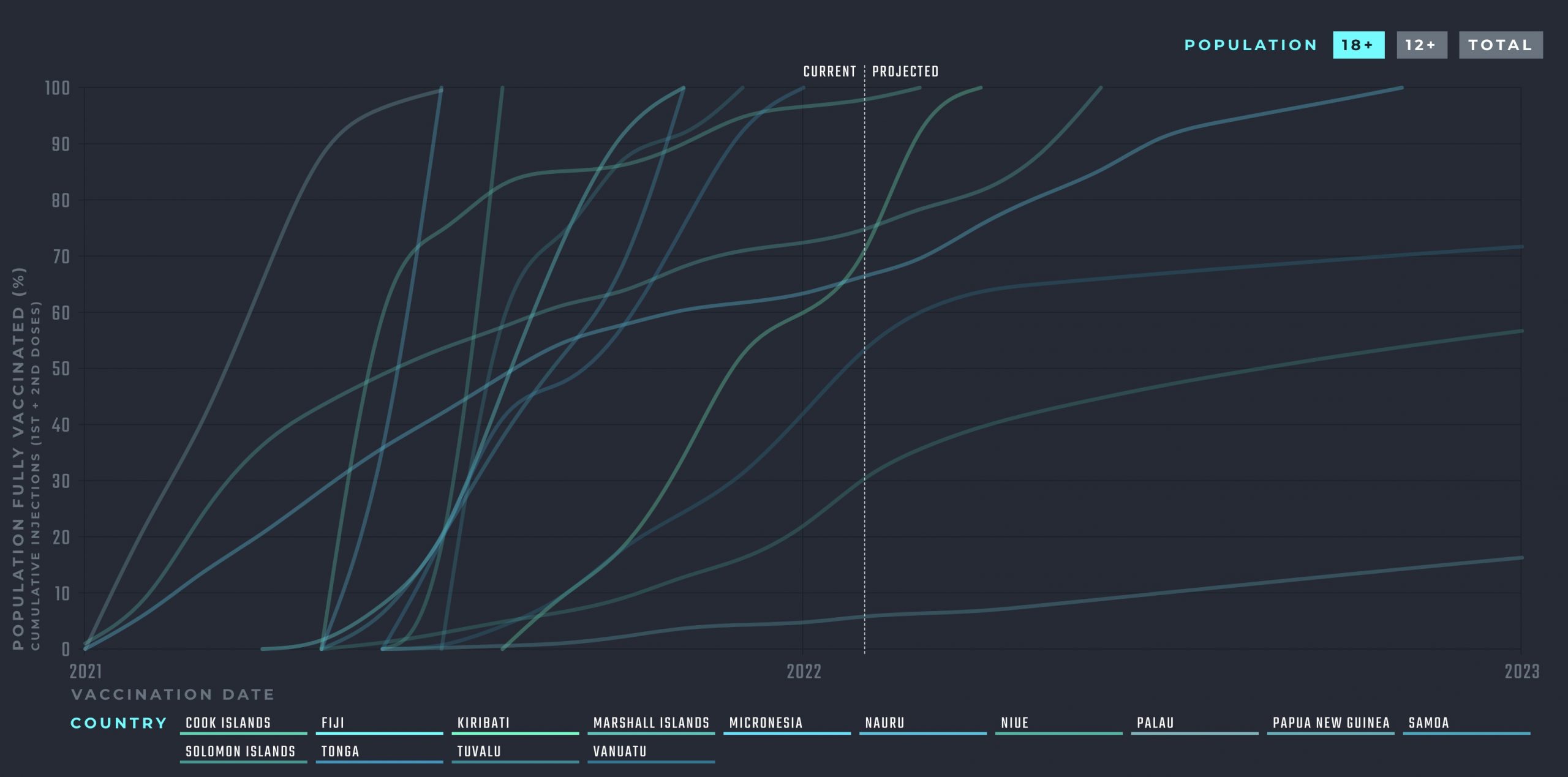
In November last year, the Lowy Institute published a model forecasting vaccine distribution across the Pacific. What it showed was a divided Pacific. Back then, many island nations – particularly the microstates such as Nauru, Niue and Palau – were world-leading in their vaccination efforts, achieving near complete vaccination coverage. Other states such as Fiji and Samoa, thanks in large part to effective rollout campaigns, looked set to achieve similar milestones by December 2021 or early 2022. Others – notably Papua New Guinea (PNG), Solomon Islands and Vanuatu – were on track to be amongst the last in the world to reach high levels of vaccination. The most concerning case was that of PNG, which our model projected would only have 35% of its adult population vaccinated by July 2026.
Fast forward five months and the picture remains almost unchanged, albeit with minor yet steady improvements. To date, half the Pacific Island countries have their adult population fully vaccinated. Kiribati, the Marshall Islands and Micronesia have all vaccinated more than 70% of their adult population and are set to reach full adult vaccination by mid-year, while Melanesian states are still lagging, with notably Solomon Islands at 32% of its adult population, and PNG at a worrying 5%.
Most Pacific nations have learnt critical lessons with respect to the requirements for rapid response, as well as the need for effective and coordinated vaccine distribution strategies. While there remain numerous unknowns and uncertainties related to the control of future pandemics, two key factors can be identified as having an important impact on the pace of vaccine distribution.
First is the number of healthcare workers involved in the vaccine rollout. While the Pacific has one of the lowest per capita rates of doctors in the world, the region mobilised its workforce, rapidly and effectively, once either the virus or vaccines to fight it had landed on their shore. Pictures of brave and committed nurses carrying refrigerated COVID-19 vaccines on their back across the dense forest of PNG made the rounds. Nonetheless, those efforts were quickly hampered by health professionals getting the virus themselves. For instance, last month in Vanuatu, the Ministry of Health affirmed it was short of frontline workers, with several either infected or being prevented from leaving quarantine, amid the spreading of the Omicron strain of COVID-19 on the main island.
Thanks to a new feature implemented into our model through a sliding scale, users can now see the impact a variation in the number of healthcare workers involved in the vaccine rollout could have on vaccination timelines across the region.
In the Country Level Data section of the model, users can select a specific country, and modify the number of healthcare workers involved in the domestic rollout by simply sliding the scale accordingly. Only countries that haven’t yet fully vaccinated their population can have their forecast altered this way. Users can also select which target population to look at (adults; adults + teenagers; total).
In the Solomon Islands, increasing the number of vaccination teams by as little as 10% would fast forward full vaccination for all adults by six months. Doubling this workforce in Vanuatu would save the country two years on its vaccine rollout forecast.
The impact of the number of healthcare workers involved in the rollout on vaccination timelines varies across countries, with a larger impact on small nations with high rates of urbanisation. However, it remains significant in all parts of the Pacific.
Vaccine acceptance is the other key factor impacting the distribution of vaccines. The state of vaccine acceptance – the inverse of vaccine hesitancy – in Melanesian countries remains low and has been a challenge even before the current pandemic. For instance, PNG’s most recent coverage survey of DTP3 – a vaccine similar in its inoculation to the COVID-19 vaccine – was only 42%, the lowest across the whole region. As such, it is not surprising that for much of the last two years the problem in Melanesia has been a lack of demand for vaccines rather than a lack of supply. Health workers deployed to vaccinate vulnerable people in the near-inaccessible part of the country report being met with solid hostility.
Vaccine acceptance rates can be improved by investing in effective and localised communication strategies to alter public, government and healthcare workers’ perceptions.
While difficult to quantify precisely, the results of our model are clear: increasing vaccine acceptance, even slightly, would dramatically shorten vaccination timelines. In the case of the Solomon Islands – which the model expects to be fully vaccinated by March 2026 – an increase in vaccine acceptance by 10% would save the country 13 months in our forecast.
Here again, users can modify vaccine acceptance settings in our model to see their effect on vaccination timelines.
Over the past two years, it has become abundantly clear that places like Papua New Guinea – where group gatherings continue despite low vaccination rates – risk facilitating the emergence of new variants with potential for immune evasion, increased disease severity, and global spread.
It is in all of our interests to limit those risks.