While the COVID-19 pandemic is a global emergency, there is another infectious airborne disease that has at best similar or arguably worse impacts and is inextricably linked to poverty and lack of access to health care – tuberculosis (TB).
TB is both preventable and curable, yet in 2019 an estimated 10 million people contracted the disease, and 1.4 million died from TB, continuing its status as the largest cause of death of any infectious disease prior to the COVID-19 pandemic.
In March 2019, The Lancet Commission on Tuberculosis concluded that the prospect of a TB-free world was a realistic objective that could be achieved with sufficient accountability and resources, and detailed the catastrophic consequences of failing to do this.
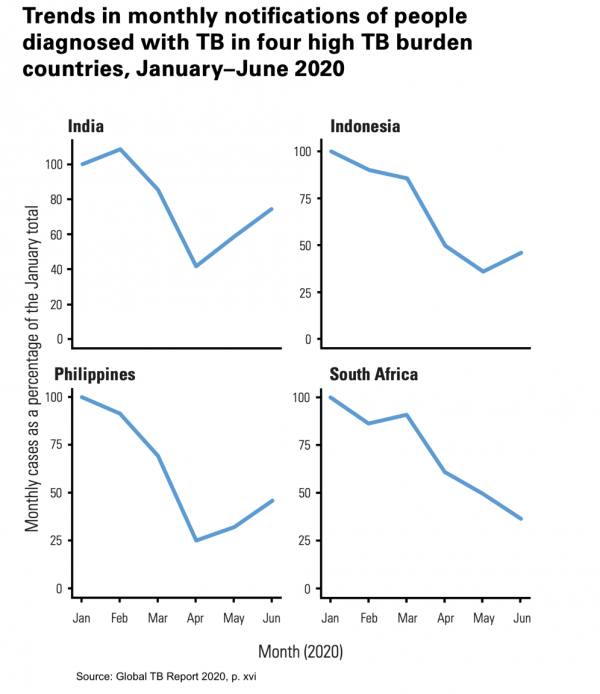
The recently released World Health Organization (WHO) Global TB Report 2020 and progress report on the implementation of the UN Political Declaration on Tuberculosis both demonstrate that most countries were making some progress in reducing the number of people falling ill with and dying from TB. However, COVID-19 has stalled and is likely to reverse this progress, with TB services including testing, treatment and prevention disrupted during the pandemic. This has already led to a reduction in the number of people diagnosed with TB in 2020, which could lead to a dramatic increase in additional TB deaths.
This blog summarises the key trends and challenges outlined in the WHO reports, and the impact and opportunities of COVID-19 on TB.
Progress towards the 2020 WHO End TB Strategy targets
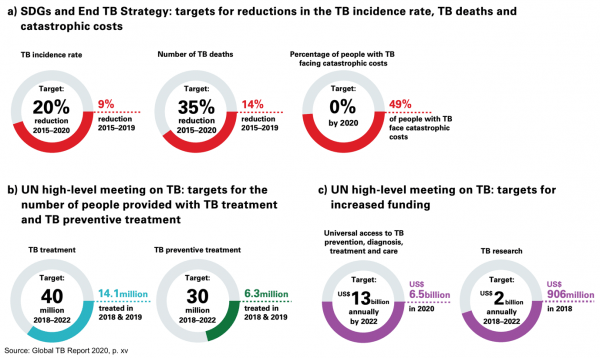
The WHO’s End TB Strategy sets out ambitious targets to reduce the number of TB cases, TB deaths and catastrophic expenses due to TB by 2035, with interim milestones set for 2020 and 2025.
Between 2015 and 2019, the following global TB trends occurred:
- The number of people newly developing TB each year fell from 142 to 130 new cases per 100,000 people globally. While 10 of the 30 high-burden countries have met or are on track to meet the 2020 WHO milestone of a 20% reduction in incidence since 2015, overall the world is not.
- The number of people dying from TB fell by 14%, but the rate is not declining quickly enough to meet the 2020 milestone of 35%.
- More people with TB are being detected by the health system, with the number of people diagnosed with TB increasing to 7.1 million in 2019, compared with 6 million in 2015. This means the number of people with TB not detected or “missed” each year has declined, probably due to investment in active case finding.
- A large proportion of people with TB face catastrophic health costs (equal to more than 20% of household income): 49% of all people with TB, and 80% of people with drug-resistant TB, faced catastrophic costs in 2019.
Shortfalls in progress towards the 2022 UN high-level meeting targets
The UN high-level meeting political declaration on TB contained targets for increasing detection, treatment and preventative treatment of TB, as well as increased funding for TB prevention and treatment programs, and TB research and development. The shortfalls against these goals include:
- 1 million people were treated for TB in 2018–19, which is only 35% of the 40 million target by 2022.
- In 2018 and 2019, 6.3 million people started TB preventive treatment, just over one-fifth of the five-year target.
- Total funding for TB prevention, detection and treatment in 2020 is estimated at US$6.5 billion, around half of the 2022 target in the political declaration.
- Research and development funding for TB was US$906 million in 2018, less than half of the 2022 target in the political declaration of US$2 billion per year.
Impacts of COVID-19
The COVID-19 pandemic is setting back progress towards ending TB in two ways:
- The health system impact, such as redirection of health resources and lockdowns, reduces access to and use of TB services.
- The economic impacts are reducing per capita incomes and increasing undernutrition, two risk factors for TB.
According to the Global TB Report, TB deaths could increase by an extra 0.2 to 0.4 million in 2020, and an extra 1 million people could develop TB per year in the 2020 to 2025 period.
How to reinstate progress on TB in the COVID-19 era
There is an excellent opportunity to leverage COVID-19 responses and recovery programs to maintain and improve TB services – including diagnostics, active case finding, contact tracing programs and digital health tools. For example, integrating population screening for TB and COVID-19 using the same workforce and testing platform. Integrating such services would not only be a smart and cost-efficient investment, but likely preferred by communities and health service providers.
Targeted public health and communications campaigns have played a key role in tackling COVID-19. For TB interventions to lead to improved health outcomes, the affected community needs to be at the centre of the response. It is crucial to involve the community in planning and priority-setting for TB resources and engage the community in developing effective health communication.
Even before the COVID-19 pandemic, TB faced a significant shortfall in funding. Delays in increasing funding will only make the response more costly in the long term. Funding for both TB services and research and development needs to be a higher priority in the national budgets of countries with high TB burdens and in official development assistance.
The Global Fund to Fight AIDS, Tuberculosis and Malaria has identified it would require an additional US$5 billion to offset the impacts of COVID-19 on the decades of progress made in the fight against HIV, TB and malaria. With international funding for most TB programs coming from the Global Fund, increased support to the Fund from donor countries is essential to resuming progress towards TB prevention, detection and treatment.
There has been a remarkable investment in COVID-19 research and development in 2020 to develop and deliver tests, treatments, vaccines, digital tools and global financing and procurement facilities to ensure equitable access (for example, the Access to COVID-19 Tools Accelerator). This demonstrates that global solidarity, political leadership, and massive resource mobilisation in science and public health, to address global development and health security are possible.
The momentum built in 2019 to galvanise ending TB needs to be re-established. As a recent article in The Lancet suggests, we can use the political capital from the COVID-19 response to build back better and meet the global commitments and targets to End TB as a global public health threat.


Leave a Comment