Few would question the urgent need to support human health responses to COVID-19 in our region; it is the right thing to do. However, while Australians may feel secure in the knowledge that this pandemic will not adversely affect national food security, the same cannot be said for many low- and middle-income countries.
Prior to the coronavirus pandemic, over 10 per cent of people globally were undernourished and approximately 30 per cent deficient in key micronutrients. Malnutrition impacts negatively on the immune system, placing the malnourished at increased risk of poorer outcomes when infected by COVID-19. Additionally, malnutrition is more prevalent in resource-limited settings and is felt unevenly within households, frequently affecting young children, women of reproductive age and the elderly. Reports from the Food and Agriculture Organization of the United Nations and UNICEF in 2019 highlighted that food and nutrition insecurity are increasingly real for millions of people. Significantly, food and nutrition security were also emphasised as a vital component of health in the 2019 United Nations Declaration on University Health Coverage. Malnutrition has multiple drivers, from poverty to climate change to food system failures to deliver safe, nourishing, affordable food. However, chronic under funding of the agricultural sector by both national governments and the international donor community is compounding the problem and will exacerbate the short- and long-term consequences of this coronavirus pandemic.
On the animal and plant health front, the services charged with disease prevention and control were tackling multiple challenges well before the coronavirus pandemic. For example, the spread of African swine fever (ASF) is causing huge mortalities in pigs and impacting severely on household food security and social obligations in Southeast Asia. The spread of this disease, for which there is no vaccine, was made easier due to the inadequate control of classical swine fever (CSF) which spread across the region over the past two decades. Despite the existence of a vaccine against CSF, inadequate funding of veterinary services prevented the effective implementation of CSF vaccination campaigns, rendering farmers accustomed to increasingly high mortality in their pig herds. When ASF arrived, all the farmers saw was more dead pigs, which, sadly, was nothing new.
The latest, and hugely worrying, plant health threat to reach Southeast Asia is the Fall Armyworm. This insect pest has eaten its way across South Asia and Southeast Asia, decimating crops leading to shortfalls in food for people and feed for intensively raised animals and has now arrived in Far North Queensland.
As countries in the region implement coronavirus control strategies, what will this mean for animal and plant health? National budgets that were already under strain will likely see movement of funds into the human health sector, further stripping sectors such as agriculture of much-needed funds. During the high pathogenic avian influenza (HPAI) H5N1 pandemic, the bulk of funding went to the human health sector and, to this day, H5N1 remains endemic in poultry in many Southeast Asian countries. Will animal health teams vaccinating against economically important diseases such as CSF and Newcastle disease (which is clinically indistinguishable from HPAI) have to cease work due to lack of funding to keep vaccinators safe and animals alive? Will plant health teams undertaking surveillance activities to determine the extent of spread of Fall Armyworm in nearby countries have to cease their activities – whether due to COVID-19 safety measures, or funding cuts, or both – enabling the insects’ relentless march eastward to continue unchecked? Quite likely. How can we learn the lessons of past pandemics such that we commit to adequately investing in animal and plant health and food safety along value chains? If we had taken this seriously after the avian influenza pandemic, we may have not only reduced the impact of coronavirus control activities on food security, we may have prevented it entirely.
More broadly, as we count the costs of inadequate disease surveillance and preparedness in the human health system, we must also factor in the drivers associated with the agricultural sector that facilitated the heightened impact of the disease. As a result of Severe Acute Respiratory Syndrome (SARS-CoV) and now COVID-19, we are all well aware of the ability of viruses that may cause no disease in animals to jump across to humans via the slaughter, sale, preparation and consumption of food from non-domesticated animal hosts. Consumer concerns in many countries in the region regarding a lack of access to affordable animal-source food (due to high animal mortality and market failure) and a lack of confidence in food safety (e.g. worries about food contamination with hormones, antibiotics or pesticide residues) frequently underlie preferences for non-domesticated animals sold through informal markets. Understanding of, and responses to, the drivers behind consumer and farmer behaviour are yet to be adequately researched and addressed.
Human health is intimately linked with animal, plant and environmental health. Systems thinking using One Health and Planetary Health lenses will be crucial to redesigning global and national systems that can keep us safe, well-nourished, healthy and actively contributing to community well-being. This period of forced physical isolation provides an opportunity to reflect on the systems that underpin our society and our vision for a sustainable development. What will be our vision of sustainable food security and nutritious food systems and their contribution to human health going forward? And what will we do to make our plans a reality at home and abroad?
Dr Robyn Alders is an Honorary Professor at the Development Policy Centre, ANU. She is also a Senior Consulting Fellow at the Centre on Global Health Security, Chatham House, UK, and Chair of the Kyeema Foundation, Brisbane, Australia.
This post is part of the #COVID-19 and international development series.

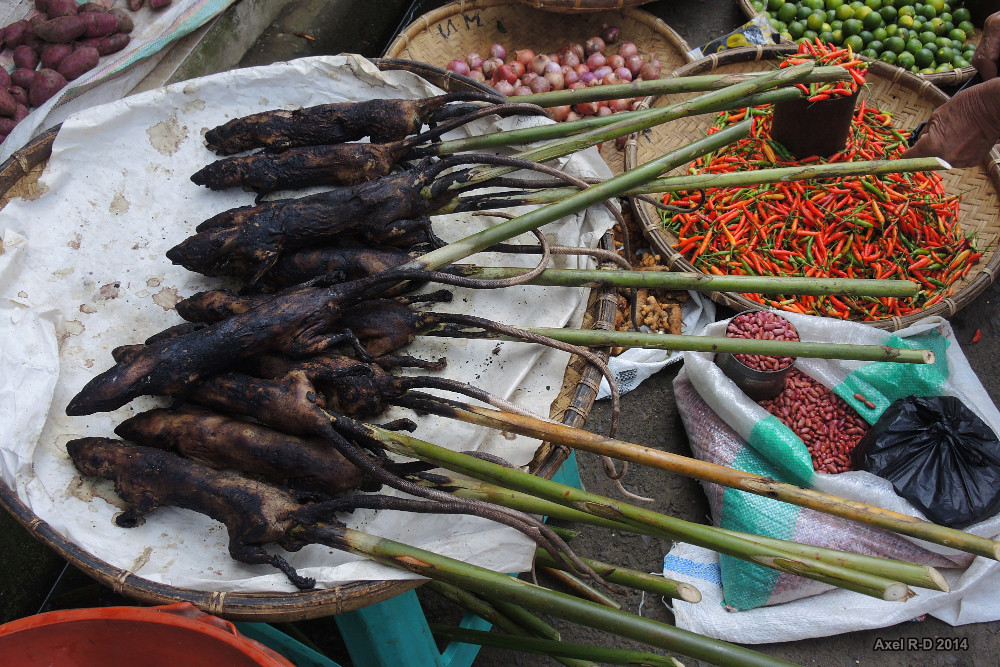






Thanks Robyn for your exemplary work. It’s my prayer that as humans we adopt systems thinking to combat these issues that are mostly affecting us with regards to GLOBAL ONE HEALTH: Towards human,animal and plant health.
I’ve shared your work with my colleagues in our department for I found it very insightful.
Be blessed always.
Thank you so much Anyonyi Octavian Jonathan for your comment. Knowing that people are thinking and talking about ways that we can work together more effectively across disciplines and sectors is really encouraging. Learning how multi- and inter-disciplinary teams are operating across different geographies will encourage and inform us all. Do please share the fruit of your discussions down the track and stay safe during these challenging times.
I have shared on LinkedIn with a comment. I think you are spot on. I have been involved in the internal plant health scene via the IPPC for many years, including as Chair of the Commission. One Health has not come up in this time and only last year we took a preliminary look at antimicrobial resistance. What do you see as the scope for plant health in One Health or other planetary initiatives?
Thanks so much Lois for your really important question. In my opinion, plant health is a key component of One Health and Planetary Health initiatives. The early vision of One Health was very holistic and getting back to this broader framework will enable us to better understand challenges and opportunities. Working together will undoubtedly prove to be much more efficient (in dollar and health terms) in the medium- to long-term. So, let’s just find a way to work together and contribute to refining definitions that will stand the test of time. I’d welcome an opportunity to learn more about your plant health endeavours.
Thank you Robyn for this constructive argument. It is a dismay how the COVID-19 turbulence will derail efforts to ensure adequate, safe and nutritious foods for all, particularly to already vulnerable food systems in low income countries. I commend you highlighting the concept of One Health/Planetary Health realizing the potential pitfall of intensifying food animal rearing on the environment and the possibility of forming a source of infection and spread of deadly pathogens with further linkage to livestock/wildlife interface and the practice of handling and consuming game animals, without forgetting the impact of agricultural expansion on the environment.
Thank you for your comments Godfrey. You are well aware of the situation on the ground in East and Southern Africa and we do hope that COVID-19 will be controlled there as quickly as possible. Thank you for your work on food safety and your commitment to improving food security in Tanzania and beyond. I agree completely with you that we do need to work together across countries and regions to ensure sustainable access to adequate, safe and nutritious foods.
Your vision is enlightening Robyn! Many thanks for exposing the real situation.
Thanks so much Kay for your comments. Let us hope that going forward we can, as Julie Garnier said below, build resilience through the regeneration of nature, gender equity and social justice.
Thanks Robyn for highlighting the increased risks of COVID-19 infection to resource-limited settings where the pandemic’s impacts will potentially be devastating. As you so rightly said, women and children are the ones already suffering the most from malnutrition and we must address and mitigate the gendered impact of the COVID-19 infection as an equal emergency during the crisis, while also building resilience through nature regeneration, gender equity and social justice in the long-term.
Thank you Julie, I couldn’t agree more with your comments.
Thanks Robyn for so eloquently describing the underlying problems of our health system, which our food systems are a part. When the dust begins to settle from the COVID-19 crisis we will need strong arguments for a review of current health policies and implementing agencies. The balance between a curative medicine and preventive surveillance and response measures has never been equal, yet this crisis highlights very strongly the need for greater understanding of the emergence of pathogens from food systems, their rapid detection and proportionate management responses.
Thank you Jonathan, for your insightful comments. I look forward to the day when farmers and public health specialists work together as co-contributors to a healthy society and preventive medicine activities receive the modest but essential support required.
Thanks for bringing up such an important topic about the intertwining effects of human health, and plant and animal health. It’s just so much to follow COVID-19 itself that sometimes we forget to look at the broader, interacting factors, and how support across these different entities will be affected. It would be good if governments can better understand that competing priorities shouldn’t be examined in a siloed fashion, but to examine them synergistically to see the larger threats to people’s health, agriculture, environment, society, and economy.
Thanks so much Holly for your future looking and positive comments. It would be great to work with you and others to increase engagement with our nation’s representatives, their teams and Australians in general to apply systems thinking to these complex problems at home and abroad.