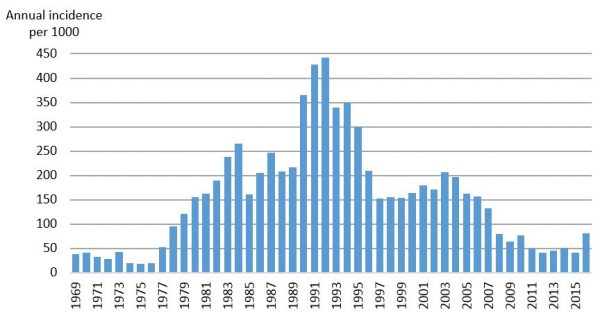
The burden of malaria in Solomon Islands remains among the highest of all countries outside of sub-Saharan Africa. But significant improvements in malaria control have been made over the last 25 years. From a peak of nearly 450 new cases per 1,000 population in 1993, by 2016 annual national malaria incidence had dropped to 81 (Figure 1).
Figure 1: National annual parasite incidence (API), 1969-2016
Data sources: 1969-1991: Over et al, 2004; 1992-2016: Ministry of Health and Medical Services, 2017
Solomon Islands is also one of the world’s most aid-dependent nations, and assistance from international donors has been particularly visible in the health sector. Foreign aid for malaria was especially prominent starting from 2003, when the Global Fund to Fight AIDS, TB and Malaria first invested in Solomon Islands, and rose again after 2007 when AusAID’s Pacific Malaria Initiative was launched, as shown in Figure 2.
Figure 2: Estimates of Solomon Islands Government (SIG) and donor contributions to malaria, 2003–2016 (US$ current)
Sources: Refer to Discussion Paper (Figure 4).
What role did this substantial influx of foreign aid play in reducing malaria in Solomon Islands, and what impact did it have on the broader Solomon Islands health system? This is the topic of our new Discussion Paper. As part of this, the paper also considers the efforts of the Solomon Islands Ministry of Health and Medical Services to coordinate donors and improve aid effectiveness, as well as its broader health system reform efforts. The findings are based on a series of in-depth, semi-structured interviews that we conducted earlier this year, as well as a review of the published and grey literature.
The first half of the paper reviews the history of malaria control and donor involvement in Solomon Islands, from the post-World War II period through to the present. The second half of the Discussion Paper presents our analysis of the impact and effectiveness of that aid, focusing on six key observations. We focus on these observations in this blog.
First, while it is difficult to establish a direct relationship between the provision of foreign aid and a specific health outcome, overall the data suggest that aid did significantly contribute to a reduction in malaria in Solomon Islands. Support from the Global Fund, which commenced in 2003, was pivotal because it enabled a substantial scaling-up of key technical interventions such as insecticide-treated bed nets, drugs, and rapid diagnostic tests. Australian aid, particularly in the period 2007 to 2016, was critical in supporting the implementation of Global Fund-funded interventions, and in providing a consistent source of funding that could be flexibly applied. There also seems to have been reasonable coordination among the various international donors funding malaria activities. However, there were also challenges. There are concerns that implementation issues within the Ministry of Health (particularly at the provincial level) were inadequately addressed, in part due to limited assessments of such challenges in grant preparation by both Global Fund and Australia.
Second, while the Global Fund and Australia now make their investments through Solomon Islands country systems, the majority of support for malaria historically has been provided in a highly vertical manner, with implementation reliant upon parallel systems used by the National Vector Borne Disease Control Program (NVBDCP). There is thus little evidence of positive spill-over from this parallel approach to the broader health system. Having developed into a highly siloed, independent program, the NVBDCP is currently faced with the challenge of reintegrating into the Ministry of Health as part of a broader integration and decentralisation reform agenda that commenced in 2011. Reintegration has been made somewhat easier by Australia’s contribution to the Health Sector Support Program (including budget support and technical assistance) since 2009, which has helped to strengthen the Ministry of Health’s supply, information and financial management systems.
Third, as donor funding reduces, sustaining the gains that have been made through the national malaria program will be dependent on strengthening the capacity of provincial malaria teams to plan, budget, and deliver interventions appropriate to their provinces. This represents a significant contrast with earlier donor support designs, which assumed a centralised model in which provincial malaria teams represented little more than ‘body shops’ to deliver bed nets and insecticide spraying. Beginning in 2016, the NVBDCP began handing over greater responsibility for implementation to Provincial Health Offices. However, this handover will be an extended process, and one which will require greater attention from donors than it has received in the past.
Fourth, while the available evidence suggests that aid was, for the most part, spent on technically effective interventions which reduced the burden of malaria in Solomon Islands, the evidence for how efficiently and cost-effectively that aid was spent is limited. Research on malaria control and elimination was one area in particular where the efficiency of spending was questioned. Although it made significant contributions to the global evidence base on malaria elimination, the high cost of research must be weighed against the need for service delivery in the Solomon Islands context.
Fifth, although the Ministry of Health previously had little ownership over the initiation and management of donor funding for malaria, since about 2012 it has worked with development partners to increase its involvement in the governance of the national malaria program. One of the key ways it has done this is to become Principal Recipient of the Global Fund grant starting from 2015. (Previously, this role was held by Pacific Community (SPC), as part of a regional grant with 10 other countries). The transition of Australian aid funding to broad health sector support has also given the Ministry of Health greater control over the use of these donor resources. The Solomon Islands government has also increasingly financed the NVBDCP, beginning in 2009.
Finally, though the political appetite for pursuing malaria elimination is resilient, history shows that achieving malaria elimination is highly challenging. In Solomon Islands, operational and health systems constraints at the provincial level, a complex geography, and the relatively high proportion of the population with G6PD deficiency (a genetic condition that complicates treatment of one type of malaria) are key barriers. For these reasons, a nuanced and evidence-informed policy dialogue on elimination will need to take place between the Ministry of Health and development partners, to determine how best to pursue elimination in a way that is cost-effective and complementary to malaria control efforts.
The findings of this paper are important first and foremost for Solomon Islands as it seeks to sustain the gains that have been made to date and continue to drive further improvements. However, the findings also have wider relevance. History shows that successes in malaria control can be fragile, with resurgence of disease as a result of reduced funding, restructuring of health systems, and changes in vector behaviour and resistance, among other causes. As global development assistance dedicated to malaria declines, many countries will be pressed to ensure the most effective use of available funds to control malaria and work towards elimination. We hope this paper illuminates some important aid effectiveness lessons for recipient and donor countries alike.
The discussion paper can be found here.









Seventh, effective change usually requires a commitment over many years?